What Does Family Planning Medicaid Cover in Nm
| Cardinal Takeaways |
|
Introduction
Many people crave fertility help to take children. This could either exist due to a diagnosis of infertility, or because they are in a same-sexual activity human relationship or single and desire children. While at that place are several forms of fertility assistance, many services are out of reach for most people because of price. Fertility treatments are expensive and oftentimes are not covered by insurance. While some individual insurance plans embrace diagnostic services, there is very fiddling coverage for treatment services such equally IUI and IVF, which are more expensive. Near people who utilise fertility services must pay out of pocket, with costs often reaching thousands of dollars. Very few states require individual insurance plans to encompass infertility services and simply i state requires coverage under Medicaid, the health coverage programme for depression-income people. This widens the gap for low-income people, fifty-fifty when they have health coverage. This brief examines how admission to fertility services, both diagnostic and treatment, varies across the U.S., based on state regulations, insurance type, income level and patient demographics.
Diagnosis and Treatment Services
Infertility is most commonly defined1 as the disability to reach pregnancy afterwards 1 year of regular, unprotected heterosexual intercourse, and affects an estimated x-fifteen% of heterosexual couples. Both female and male factors contribute to infertility, including problems with ovulation (when the ovary releases an egg), structural bug with the uterus or fallopian tubes, problems with sperm quality or move, and hormonal factors (Effigy 1). Most 25% of the time, infertility is acquired by more than than one factor, and in virtually 10% of cases infertility is unexplained. Infertility estimates, however exercise not account for LGBTQ or single individuals who may also need fertility assistance for family unit edifice. Therefore, there are varied reasons that may prompt individuals to seek fertility care.

Figure 1: In that location Are Multiple Reasons Someone May seek Fertility Assistance
A broad array of diagnostic and treatment services may be necessary to assist in fertility (Table one). Diagnostics typically include lab tests, a semen assay and imaging studies or procedures of the reproductive organs. If a likely cause of infertility is identified, handling is ofttimes directed at addressing the source of the problem. For example, if someone has abnormal thyroid hormone levels, thyroid medications may aid the patient attain pregnancy. If a patient has big fibroids distorting the uterine cavity, surgical removal of these benign tumors may allow for futurity pregnancy. Other times, other interventions are needed to assistance the patient achieve pregnancy. For example, if a semen assay reveals poor sperm motility or the fallopian tubes are blocked, the sperm will not exist able to fertilize the egg, and intrauterine insemination (IUI) or in-vitro fertilization (IVF) may be necessary. These procedures besides facilitate family unit edifice for LGBTQ and single individuals, with utilise of donor egg or sperm, with or without a gestational carrier (surrogacy).
| Table 1: Overview of Common Fertility Services | |
| Diagnostic Services: |
|
| Treatment Services: |
|
| Fertility Preservation: |
|
| NOTES: This is not an exhaustive list of infertility services. SOURCE: ACOG. Evaluating Infertility. 2017; ACOG. Treating Infertility. 2019; American Society for Reproductive Medicine. Infertility: An Overview. Patient Information Serial. 2017 | |
Utilization of Fertility Services
Our analysis of the 2015-2017 National Survey of Family unit Growth (NSFG) finds that 10% of women2 ages xviii-49 say they or their partner have ever talked to a doctor about means to help them get pregnant (information not shown).3 Among women ages 18-49, the virtually commonly reported service is fertility advice (Figure 2).
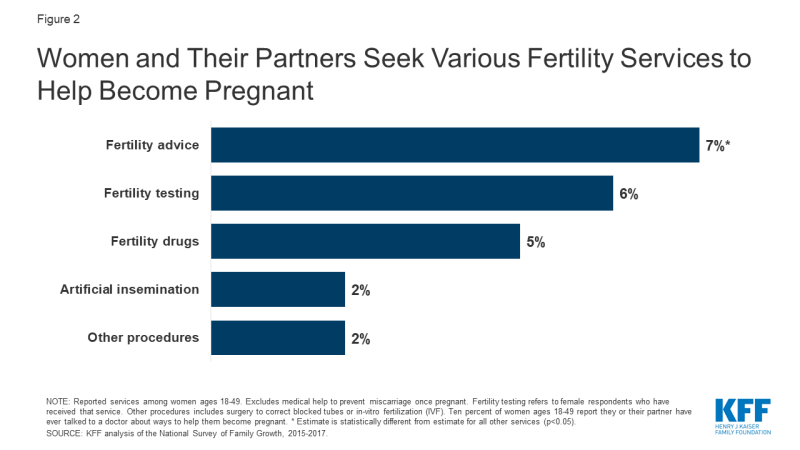
Figure 2: Women and Their Partners Seek Various Fertility Services to Help Become Pregnant
The CDC finds that employ of IVF has steadily increased since its first successful nascency in 1981. According to the nigh recent data, an estimated one.8% of U.S. infants are conceived annually using assisted reproductive technology (ART) (e.g., IVF and related procedures).4 The proportions are highest in the Northeast (MA 4.vii%, CN 3.9%, NJ 3.ix%), and lower in the Southward and Southwest (NM 0.4%, AR 0.6%, MS 0.half-dozen%).
Utilization of fertility services has dropped drastically during the COVID-19 public health emergency. On March 17, 2020 the American Gild for Reproductive Medicine (ASRM) issued guidelines to finish all new fertility treatment cycles and not-urgent diagnostic procedures. Since then, ASRM has provided updated guidance on what conditions should be met and measures should be taken before safely resuming fertility care. During this time, a study by Strata Decision Technology of 228 hospitals across xl states establish patient encounters for infertility services were down 83% from March 22 to April four, 2020 compared to this time the year prior.
Cost of Services
Many patients lack access to fertility services, largely due to its high price and limited coverage by private insurance and Medicaid. Every bit a result, many people who use fertility services must pay out of pocket, even if they are otherwise insured. Out of pocket costs vary widely depending on the patient, state of residence, provider and insurance programme. Generally, diagnostic lab tests, semen analysis and ultrasounds are less expensive than diagnostic procedures (east.g., HSG) or surgery (eastward.g., hysteroscopy, laparoscopy). Meanwhile handling using fertility medications is less expensive than IUI and IVF, but even the less costly treatments can all the same issue in thousands of dollars of out of pocket costs. Many people must effort multiple treatments before they or their partner can attain a pregnancy (typically medication first, followed past surgery or fertility procedures if medications are unsuccessful). A report of virtually 400 women undergoing fertility care in Northern California demonstrates this overall trend, with the everyman out of pocket spending on treatment with medication only and the highest costs for IVF services (Figure 3). Prior research showed the price of only 1 standard cycle of IVF was approximately $12,500 in 2009, only is likely higher today due to rising health care costs overall. Furthermore, many patients require several rounds of handling before achieving a pregnancy, with costs accruing each cycle making these interventions financially inaccessible for many. In addition to costs for the bodily treatment, patients can be saddled with out of pocket expenses for office visits, diagnostic tests/procedures, genetic testing, donor sperm/egg apply and storage fees and wages lost from time off work.
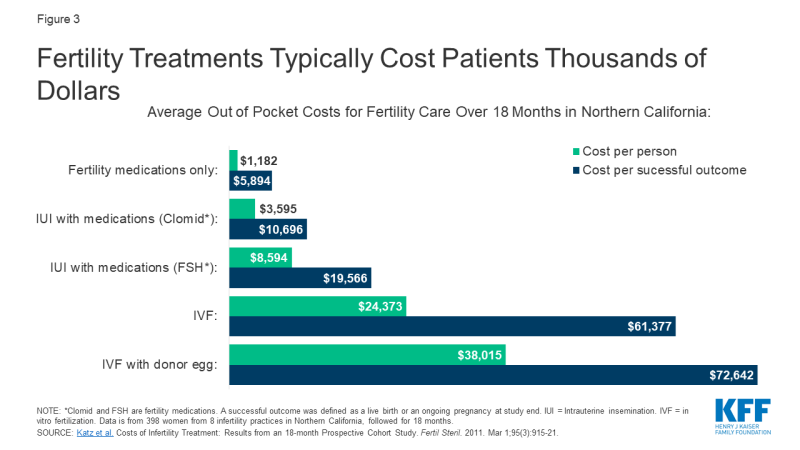
Figure 3: Fertility Treatments Typically Cost Patients Thousands of Dollars
Insurance Coverage
Insurance coverage of fertility services varies by the state in which the person lives and, for people with employer-sponsored insurance, the size of their employer. Many fertility treatments are not considered "medically necessary" past insurance companies, so they are non typically covered by individual insurance plans or Medicaid programs. When coverage is available, certain types of fertility services (due east.yard., testing) are more likely to be covered than others (e.g., IVF). A handful of states require coverage of fertility services for some fully-insured private plans, which are regulated past the state. These requirements, still, do not apply to health plans that are administered and funded directly past employers (self-funded plans) which cover six in ten (61%) workers with employer-sponsored wellness insurance. States likewise accept purview over the benefits covered by their Medicaid programs. The federal government has authority over benefit requirements in federal health coverage programs, including Medicare, the Indian Wellness Service (IHS) and military health coverage.
Individual Insurance
Xv states take laws in consequence requiring sure health plans to cover at least some infertility treatments (a "mandate to cover") (Figure 4). Additionally, Colorado recently enacted a requirement for individual and group health do good plans to cover infertility diagnosis, treatment and fertility preservation for iatrogenic infertility, effective Jan 2022. Among states that practice not have a mandate to cover, 9 states5 and DC take a criterion plan that includes coverage for at least some infertility services (diagnosis and/or treatment) for about individual and small-scale group plans sold in that state.vi 2 states (CA and TX7) require group health plans to offer at least ane policy with infertility coverage (a "mandate to offer"), but employers are not required to cull these plans.
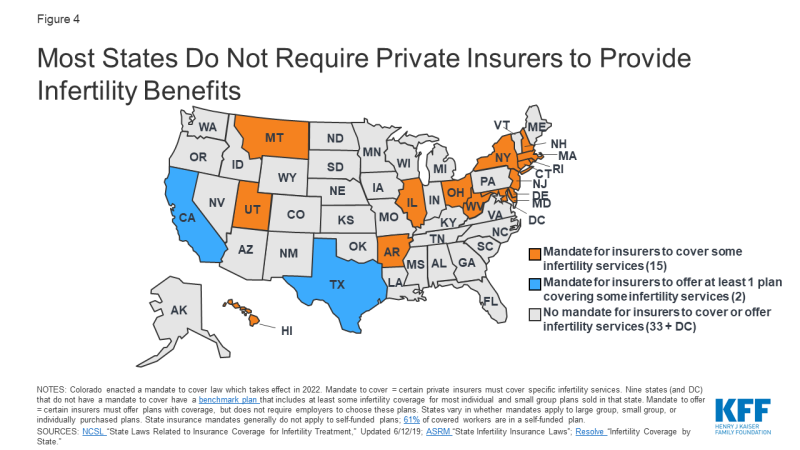
Effigy 4: Most States Do Not Crave Individual Insurers to Provide Infertility Benefits
However, in states with "mandate to cover" laws, these only apply to certain insurers, for certain handling services and for certain patients, and in some states have monetary caps on costs they must cover (Appendix 1). For case, in OH and WV, the requirement to embrace infertility services simply applies to wellness maintenance organizations (HMOs). In other states, almost all insurers and HMOs are included in the mandate. Many states provide exemptions for small-scale employers (<fifty employees) or religious employers. In addition, land laws do not apply to self-funded (or cocky-insured) employer plans, which are regulated by federal law. 60-one percent of covered workers are enrolled in a self-funded programme.
Even in states with coverage laws, non all patients are eligible for infertility treatment. In Hi, someone with unexplained infertility just qualifies for IVF after five years of infertility. In others, patients are eligible after 1 year. Some states place age limits on female person patients who can access these services (e.chiliad., ineligible if 46 or older in NJ or if under age 25 or older than 42 in RI). Others identify restrictions based on marital status; for example, until May 2020, IVF benefits were simply bachelor to married women in Doc. Recently enacted legislation now expands coverage to single women. Additionally, it is not always made clear if LGBTQ individuals meet eligibility criteria for these benefits, without a diagnosis of infertility. Furthermore, many costs associated with surrogacy are often not covered by insurance.
States also vary in which treatment services they require plans to cover. Some states mandate insurers to cover cryopreservation for persons with iatrogenic infertility, while others do not. Four states with insurer mandates do not comprehend IVF. Eleven states exercise, simply with a dollar limit on coverage (e.g., $15,000 lifetime max in AR and $100,000 in MD and RI) or a limit on the number of cycles they will encompass (e.g., 1 cycle of IVF in Hullo and three cycles in NY).
Do land mandates for IVF coverage affect use of services?
IVF utilization appears to be higher in states with mandated IVF coverage. CDC information from 2016 showed that in three of the 4 states deemed past the CDC to have "comprehensive coverage"viii for IVF (IL, MA, NH), apply of assisted reproductive engineering was ane.5 times higher than the national rate. Similarly, a national report found that IVF availability and utilization9 were significantly higher in states with mandated IVF coverage. A study in MA institute IVF utilization increased later on implementation of their IVF mandate, but overutilization by patients with a low chance of pregnancy success was not found. State level mandates tin also help reduce inequities in access. For example, a contempo bill proposed in the CA legislature would reverse existing limitations on fertility coverage and brand the do good bachelor to single women and women in same sexual practice relationships.
What does it cost to cover fertility benefits?
While the costs of fertility treatments can be very expensive for those who lack coverage, the cost of roofing fertility benefits varies depending on the services covered and utilization with implications for country budgets, employers, and policy holders. For instance, in 2019, New York passed a beak to require IVF and fertility preservation services for comprehensive private health insurance policies. The New York State Department of Fiscal Services estimated that premiums would increase 0.5% to 1.one% due to mandating IVF coverage, and 0.02% for mandating fertility preservation for iatrogenic infertility (acquired past medical treatments).
An assay of a bill proposed in CA to require private plans and Medi-Cal managed care plans to cover IVF services estimated that per fellow member per calendar month premiums would increase by approximately $5 in the private market and less than a $1.00 for Medi-Cal plans. Overall though, out of pocket spending for individuals seeking services would subtract substantially.
Data from MA, CT and RI suggest that mandating coverage does not announced to enhance premiums significantly. All 3 states take been mandating infertility benefits for over 30 years, and judge the cost of infertility coverage to be less than 1% of total premium costs. In 2017, California was considering a more limited bill that would require fertility preservation for iatrogenic infertility in certain individual and group health plans. As the neb was introduced, it was estimated to result in a net annual increase of $2,197,000 in premium costs or 0.0015% for enrollees in plans subject area to the mandate.
While these costs could be small-scale in comparison to the costs of paying out-of-pocket for these services, at that place are other costs to coverage mandates. The ACA requires states to get-go some of the costs for any land mandated benefits beyond essential wellness benefits (EHBs) in the individual and small group market. This requirement was estimated to toll NY $59 to $69 million per yr if covering i cycle or $98 to $116 meg per twelvemonth if covering unlimited cycles of IVF.
What share of employers offer fertility benefits?
Large employers are more likely than smaller employers to include fertility benefits in their employer-sponsored health plans. According to Mercer'due south 2017 National Survey of Employer-Sponsored Wellness Plans, 56% of employers with 500 or more than employees cover some type of fertility service, but most do non encompass treatment services such as IVF, IUI, or egg freezing. Coverage is higher for diagnostic evaluations and fertility drugs. Coverage is more common among the largest employers and those that offer higher wages (Effigy five).
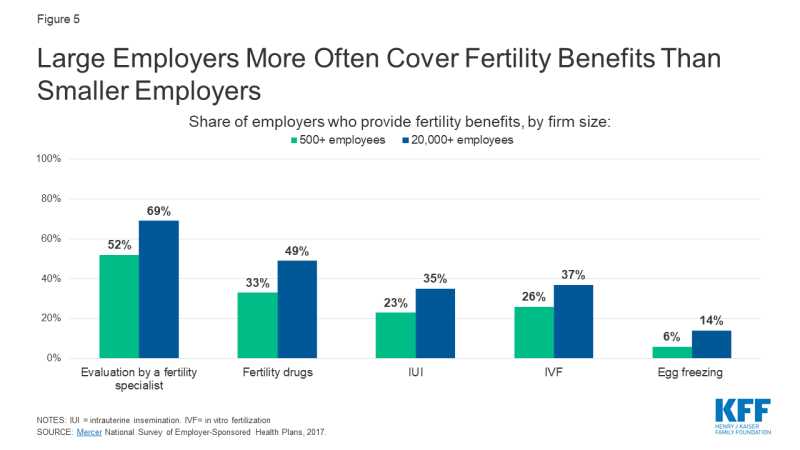
Figure 5: Large Employers More Often Encompass Fertility Benefits Than Smaller Employers
Public Coverage
Medicaid
NSFG data show that significantly fewer women with Medicaid have always used medical services to aid become pregnant compared to women with individual insurance. Every bit of January 2020, our analysis of Medicaid policies and benefits reveal merely 1 state, New York, specifically requires their Medicaid program to comprehend fertility treatment (limited to 3 cycles of fertility drugs) (Figure 6). However, some states may require Medicaid to cover treatments for conditions that touch on fertility, while non direct stated in their policies. For instance, states may cover thyroid medications, or cover surgery for fibroids, endometriosis or other gynecologic abnormalities if causing pelvic pain, aberrant bleeding or another medical trouble, other than infertility. No state Medicaid program currently covers artificial insemination (IUI), IVF, or cryopreservation (Appendix 2).
Some states specifically cover infertility diagnostic services; GA, Hello, MA, MI, MN, NH, NM and NY all offer at least one Medicaid plan with this do good, only the range of diagnostics covered varies. For case, New York Medicaid specifically covers role visits, HSGs, pelvic ultrasounds and claret tests for infertility. Meanwhile, the infertility cess covered by Georgia Medicaid includes lab testing, but not imaging or procedural diagnostics. Other states specifically do not cover infertility diagnostics, or more mostly exercise not encompass "infertility services," which likely includes diagnostics. Others do not mention infertility diagnostics in their Medicaid policies, significant the beneficiary would need to cheque with their Medicaid programme to run into if these services are covered (Appendix ii).
The Medicaid program's lack of coverage of fertility aid has a disproportionate impact on women of colour. Amidst reproductive age women, the plan covers three in ten (30%) who are Black and one quarter who are Hispanic (26%), compared to 15% who are White. Because eligibility for Medicaid is based on beingness low-income, people enrolled in the program likely could not beget to pay for services out of pocket.
The relative lack of Medicaid coverage for fertility services stands in stark contrast to Medicaid coverage for maternity care and family planning services. About half of births in the U.S. are financed by Medicaid, and the program finances the majority of publicly-funded family planning services. Therefore, while there is wide coverage of many services for low-income people during pregnancy and to aid prevent pregnancy, there is almost no access to help low-income people achieve pregnancy.

Figure half-dozen: Ane State Medicaid Programme Covers Infertility Treatment and Viii Cover Some Diagnostics
Medicare
While most beneficiaries of Medicare are over the age of 65+, Medicare also provides health insurance to approximately ii.five one thousand thousand reproductive historic period adults with permanent disabilities. According to the Medicare Benefit policy manual, "reasonable and necessary services associated with treatment for infertility are covered under Medicare." However, specific covered services are not listed, and the definition of "reasonable and necessary" are not defined.
Military
TRICARE: TRICARE, the insurance program for military families, volition comprehend some infertility services, if deemed "medically necessary" and if pregnancy is achieved through "natural conception," pregnant fertilization occurs through heterosexual intercourse. Diagnostic services are covered, including lab testing, genetic testing, and semen analysis. Treatment to correct physical causes of infertility are as well covered. Withal, IUI, IVF, donor eggs/sperm and cryopreservation are non typically covered, unless the service member had a serious injury while on agile duty resulting in infertility.
Veterans Affairs (VA): Infertility services are covered by the VA medical benefits packet, if infertility resulted from a service-connected status. This includes infertility counseling, claret tests, genetic counseling, semen analysis, ultrasound imaging, surgery, medications and IVF (as of 2017). Even so, the couple seeking services must be legally married, and the egg and sperm must come from said couple (finer excluding aforementioned sex couples). Donor eggs/sperm, surrogacy or obstetrical care for non-Veteran spouses are non covered.
Infertility Services In Publicly Funded Clinics
The CDC's and Office of Population Affairs' (OPA) Quality Family Planning recommendations address provision of bones infertility services. Family planning providers are recommended to provide at minimum patient educational activity almost fertility and lifestyle modifications, a thorough medical history and physical exam, semen analysis, and if indicated, referrals for lab testing of hormone levels, boosted diagnostic tests (endometrial biopsy, ultrasound, HSG, laparoscopy) and prescription of medications to promote fertility. Nonetheless, studies of publicly funded family planning clinics suggest that availability of infertility services is uneven. In a 2013-2014 report of 1615 publicly funded clinics, a loftier share reported offering preconception care (94% for women and 69% for men), but fewer offered any basic infertility services (66% for women and 45% for men). Provision of whatsoever infertility treatment was uncommon (16% of clinics), likely requiring referrals to specialists who may not have Medicaid or uninsured patients.x The majority of patients who rely on publicly funded clinics are low-income and would non probable be able to afford infertility services and treatments one time diagnosed.
Per the Indian Health Services (IHS) provider transmission, basic infertility diagnostics should be made available to women and men at IHS facilities, including a history, physical exam, basal temperature charting (to predict ovulation), semen analysis and progesterone testing. In facilities with OBGYNs, HSG, endometrial biopsy and diagnostic laparoscopy should also be bachelor. However, it is unclear how accessible these services are in exercise, and provision of infertility treatment is non mentioned.
Key Populations
Racial and ethnic minorities
The ability to accept and intendance for the family that you lot wish for is a fundamental tenet of reproductive justice. For those who need it, this includes access to fertility services. The share of racial and indigenous minorities who utilise medical services to help become pregnant is less than that of non-Hispanic White women, despite research that has establish higher rates of infertility among women who are Black and American Indian / Alaska Native (AI/AN). Our analysis of 2015-2017 NSFG data shows that while xiii% of non-Hispanic White women reported ever going to a medical provider for assist getting significant, just 6% of Hispanic women and 7% of non-Hispanic Black women did so (Effigy vii). A higher share of Black and Hispanic women are either covered past Medicaid or uninsured than White women and more women with individual insurance sought fertility help than those with Medicaid or the uninsured. A variety of factors, including differences in coverage rates, availability of services, income, and service‐seeking behaviors, affect access to infertility care. Furthermore, other societal factors also play a role. Misconceptions and stereotypes nigh fertility have frequently portrayed Black women every bit not requiring fertility assistance. Combined with the history of discriminatory reproductive care and harm inflicted upon many women of color over decades, some may delay seeking infertility care or may non seek it at all.
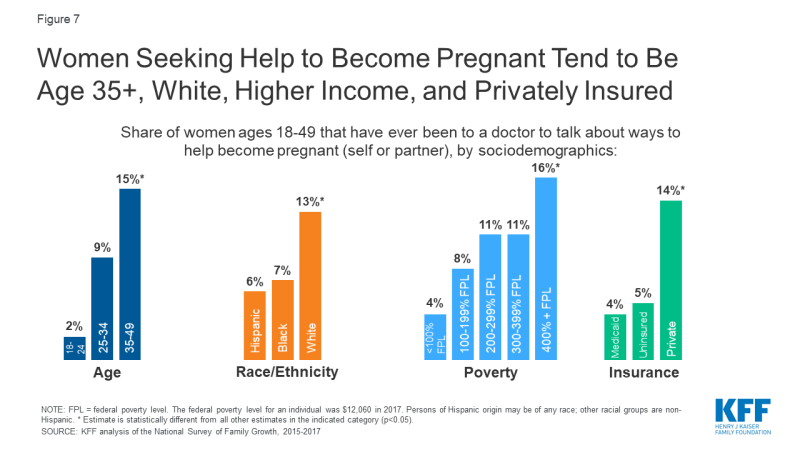
Figure vii: Women Seeking Aid to Get Pregnant Tend to Be Age 35+, White, Higher Income, and Privately Insured
Other enquiry has found that utilize of fertility testing and treatment also varies past race. An analysis of NSFG information establish that among women who reported using medical services to help become pregnant, similar shares of Black (69%), Hispanic (70%) and White (75%) women received fertility advice. However, less than one-half (47%) of Black and Hispanic women who used medical services to get pregnant reported receiving infertility testing, compared to 62% of White women, and even fewer women of color received treatment services. According to an analysis of surveillance data of IVF services, use is highest amidst Asian and White women and everyman among American Indian / Alaska Native (AI/AN) women. Racial inequities may be for fertility preservation as well; a study of female patients in NY with cancer found disproportionately fewer Black and Hispanic patents utilized egg cryopreservation compared to White patients. On average, more Black, Hispanic, and AI/AN people live beneath the federal poverty level than people who are White or of Asian/Pacific Islander descent. The high cost and limited coverage of infertility services make this care inaccessible to many people of color who may desire fertility preservation, merely are unable to afford information technology.
Iatrogenic Infertility
Iatrogenic, or medically induced, infertility refers to when a person becomes infertile due to a medical procedure done to treat another problem, almost oft chemotherapy or radiations for cancer. In these situations, persons of reproductive age may desire hereafter fertility, and may opt to freeze their eggs or sperm (cryopreservation) for later use. The American Society for Reproductive Medicine (ASRM) encourages clinicians to inform patients most fertility preservation options prior to undergoing treatment likely to cause iatrogenic infertility.
However, the toll of egg or sperm retrieval and subsequent cryopreservation tin can exist prohibitive, especially if in the absence of insurance coverage. Only a handful of states (CT, DE, IL, MD, NH, NJ, NY, and RI) specifically crave private insurers to comprehend fertility preservation in cases of iatrogenic infertility. No states currently crave fertility preservation in their Medicaid plans.
LGBTQ populations
LGBTQ people may face heightened barriers to fertility care, and bigotry based on their gender identity or sexual orientation. Section 1557 of the Affordable Care Deed (ACA) prohibits discrimination in the health intendance sector based on sexual activity, but the Trump Administration has eliminated these protections through regulatory changes. Without the explicit protections that take been dropped in the current rules, LGBTQ patients may be denied health care, including fertility care, under religious freedom laws and proposed changes to the ACA. All the same, these changes are being challenged in the courts because they conflict with a recent Supreme Court decision stating that federal civil rights law prohibits bigotry based on sexual orientation and gender identity.
In a commission opinion, ASRM concluded it is the ethical duty of fertility programs to treat gay and lesbian couples and transgender persons, equally to heterosexual married couples. They write that assisted reproductive therapy should not be restricted based on sexual orientation or gender identity, and that fertility preservation should be offered to transgender people before gender transitions. This allows transgender individuals the ability to have biological children in the futurity if desired. Despite this recommendation, in aforementioned states with mandated fertility preservation coverage for iatrogenic infertility, it remains unclear if this do good extends to transgender individuals, whose gender affirming care tin can result in infertility. Additionally, many land laws regarding mandates for infertility treatment contain stipulations that may exclude LGBTQ patients. For example, in Arkansas, Hawaii and Texas and at the VA, IVF services must employ the couple's own eggs and sperm (rather than a donor), effectively excluding same sex activity couples. In other states, aforementioned-sexual practice couples do not meet the definition of infertility, and thus may non qualify for these services. Information are defective to fully capture the share of LGBTQ individuals who may utilize fertility assistance services. Research studies on family building are frequently not designed to include LGBTQ respondents' fertility needs.
Single Parents
Single persons are often excluded from admission to infertility handling. For example, the aforementioned IVF laws cited above that require the couple's own sperm and egg, effectively exclude single individuals besides, equally they cannot use donors. Some grants and other financing options also stipulate funds must become towards a married couple, excluding single and unmarried individuals. This is in opposition to the ASRM committee opinion, which states that fertility programs should offer their services to single parents and unmarried couples, without bigotry based on marital condition.
Looking Forward
On a federal level, efforts to pass legislation to require insurers to cover fertility services are largely stalled. The proposed Access to Infertility Handling and Care Act (60 minutes 2803 and South 1461), which would crave all wellness plans offered on group and individual markets (including Medicaid, EHBP, TRICARE, VA) to provide infertility treatment, is still in committee (and never made it out of committee when proposed during the 115th congress). In that location has been some more motion on the state level. Some states require private insurers to cover infertility services, the near recent of which was NH in 2020. Currently, NY continues to be the kickoff and but state Medicaid program to comprehend any fertility treatment.
For those who desire to have children, obtaining fertility care can exist a stressful process. Stigma around infertility, intensive and sometimes long or painful treatment regimens, and uncertainty nigh success tin take a toll. On top of that, in the absence of insurance coverage, infertility intendance is toll prohibitive for most, particularly for low-income people and for more than expensive services, like IVF or fertility preservation. Pregnant disparities exist within access to infertility services across, dictated by state of residence, insurance plan, income level, race/ethnicity, sexual orientation and gender identity. Achieving greater disinterestedness in access to fertility intendance will likely depend on addressing the needs faced by low-income persons, people of color and LGBTQ persons in fertility policy and coverage.
Source: https://www.kff.org/womens-health-policy/issue-brief/coverage-and-use-of-fertility-services-in-the-u-s/
Posting Komentar untuk "What Does Family Planning Medicaid Cover in Nm"